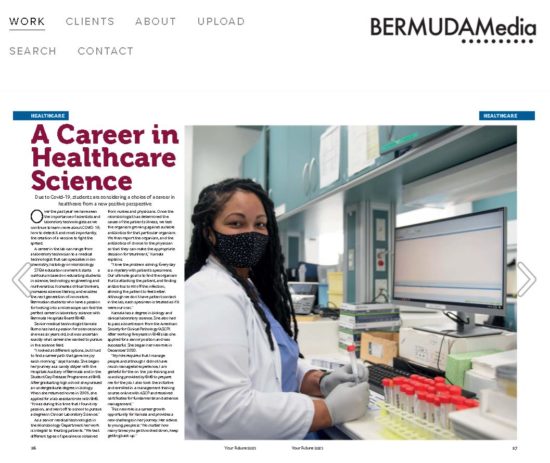
A Career in Healthcare Science
February 2021: Due to Covid-19, students are considering a choice of a career in healthcare from a new perspective
Over the past year we have seen the importance of scientists and laboratory technologists as we continue to learn more about COVID-19;how to detect it and most importantly, the creation of a vaccine to fight the spread.
A career in the lab can range from a laboratory technician to a medical technologist that can specialise in bio-chemistry, histology or microbiology.
STEM education is where it starts – a curriculum based on educating students in science, technology, engineering and mathematics. It creates critical thinkers, increases science literacy and enables the next generation of innovators…
To read the full article in Your Future Magazine February 2021 click here and go to page 26.